Janice Verdin had no illusions about how bad a nursing home could get. Over her decade and a half as a nurse in south Louisiana, she’d worked in facilities infested with roaches and vermin, buildings where mold took over and staff worked under leaking ceilings. But she felt devoted to the residents, many of whom were poor Medicaid recipients with chronic health conditions. It could be a dirty job, but someone had to do it.
By the summer of 2021, she had spent three years working at South Lafourche Nursing and Rehab — a facility in Verdin’s bayou hometown of Cut Off, owned by an eccentric millionaire named Bob Dean. Verdin had worked at Dean’s nursing homes before and found them substandard, but South Lafourche was different: The building was cleaner; the management was professional; and the other nurses cared deeply about their work. So much did it stand out from the others, Verdin said, that earlier that year she brought her aunt, Marie Roussel, there to live. She had little reason to suspect that the greatest challenge of her career was yet to come.
On the last Friday in August, the nurses knew that a serious tropical storm was headed for Cut Off; meteorologists had christened it Ida. When Verdin finished her shift the day before, her boss told her the plan was to shelter in place and weather the storm, which did not yet qualify as a hurricane. At 1 a.m., however, she was awakened by a text message that said they’d be evacuating. Dean was sending residents from all seven of his nursing homes to a building he owned in Independence, a town 100 miles north that sat well outside the storm’s projected path. Verdin was assured that everyone would be well taken care of: The administrators promised there would be catering at the warehouse, and nurses would be making at least $2,000 a day.

But when Verdin arrived in Independence around 5 or 6 p.m. on that Friday, she was unnerved by what she could see from the parking lot: The warehouse looked abandoned, with rust stains on the walls and overgrown grass all around. Inside, portable toilets were arrayed beside the dining area. There were only two sinks. The hundreds of mattresses on the concrete floor left almost no space to walk.
Verdin was also troubled to see that no one was taking precautions to mitigate the spread of COVID-19, even though Louisiana’s case rate had recently reached an all-time high. At South Lafourche, no one could enter without answering a list of questions, having their temperature taken, and putting on a mask. Those measures had clearly been discarded, even as hundreds of vulnerable people were being packed closer than ever.
Verdin’s boss rented a hotel room for himself and another for the South Lafourche nurses. They were invited to sleep there in shifts. But Verdin stayed that night in the warehouse; she wanted to be near Roussel. She claimed a mattress near the wall and put on fresh sheets. The fluorescent lights overhead couldn’t be cut off without disabling the air conditioning, thanks to a glitch in the wiring. Verdin tossed and turned most of the night. What if it starts flooding? she remembers thinking. What are we going to do?
The next day, Verdin and the other nurses kept an eye on the TV and followed the news on their phones. The storm had rapidly intensified over the the Gulf of Mexico, thanks to unusually high ocean surface temperatures, and transformed into a Category 2 hurricane, with wind speeds over 100 miles per hour. The governor, John Bel Edwards, declared a state of emergency, and New Orleans Mayor LaToya Cantrell called for an evacuation within the city limits. Edwards warned that the storm’s threat was no longer limited to the state’s coast. “I don’t want folks who are further inland to be caught off guard,” he said.
At the warehouse, the staff were apprehensive. Now that everyone had arrived, there were nearly 850 residents between the main building and an annex. The promised catering never arrived, and though there was food available — cans of ravioli, cases of hot dogs — it wasn’t enough to go around. Plus, the meal prep area was right next to the portable toilets, diminishing many appetites. Verdin conserved the Slim Jims and Little Debbie cakes she’d brought for herself and her aunt, unsure of how long they would need to last.
Some residents were becoming manic. Even in the best of circumstances, many had trouble distinguishing between day and night. Now that the lights couldn’t be turned off, they were more confused than ever. Meanwhile, the portable toilets were starting to overflow. Verdin and her colleagues established a makeshift bathroom for the residents under their care: Another nurse, Mary Helmer, found a shower chair, and they positioned it over a bucket lined with a garbage bag and kitty litter. They put up a curtain for privacy. When the nurses themselves had to go, they retreated to the parking lot and crouched beside their cars.
By Sunday evening it was clear that Independence, far from being outside of Ida’s path, was on track to be hit as hard as any part of Louisiana. Forecasters predicted 10 or more inches of rainfall in the town and wind speeds of 140 mph — significantly higher than even those brought by Hurricane Katrina in 2005. Verdin’s brother was sending her updates, saying Ida might be a Category 4 storm by the time it hit.

Just after midnight, the hurricane’s arrival was announced by the sound of the wind and the pounding of the rain. Verdin heard a scraping noise overhead. “What is that?” she asked a colleague. Branches, torn from trees, were being blown across the roof. Water was pouring down the walls, according to Helmer. The lights flickered on and off until backup generators were deployed. The air conditioner shut down for good.
When the rain and wind died down, Verdin, Helmer, and their colleagues went to check on the secondary building. Water had flooded in, and it was pooling so high off the ground that many mattresses were floating. The nurses moved the annex’s residents to the main building, but there was nowhere for them to lie down; their mattresses were ruined, soaking wet, so the nurses sat the residents up on chairs instead. Verdin did not sleep again that night.
By the next day, the facility was running out of potable water, and patients were showing signs of dehydration, becoming tired, dizzy, and confused. Oxygen tanks and diapers were also in short supply. Nurses found boxes to prop up residents’ upper bodies on their mattresses, so they’d at least get better airflow. But the ones who had lost their mattresses weren’t able to lie down again. Several patients had been taken to the hospital. By the end of the week, at least five residents would die; the total would triple in the weeks to follow. Others would develop gangrene.
In the 92-degree heat, the smell from the overflowing toilets was becoming unbearable. Verdin was wearing two masks, but whenever she reentered the warehouse after being outside, she almost choked from the odor. Many of her colleagues were vomiting.

At the warehouse where South Lafourche residents were sent in Independence, Louisiana, fluorescent lights overhead couldn’t be cut off. Janice Verdin
Verdin and Helmer both say that one manager started giving morphine to patients whom it hadn’t been prescribed to, to calm them down. The manager called herself “Mr. Sandman.” Verdin confronted her.
“If I find out you give my aunt anything that is not ordered for her,” Verdin said, “that’s going to be the last mistake you make. I will turn you in to the board.”
The rest of Verdin’s family had evacuated to Houston, and she called them throughout the day. “I can’t keep doing this,” she told them. “This is scary. Our patients are going to start to die.”
Quinn Ward, her partner, suggested that she might be overreacting.
“Janice,” he told her, “you’re making $2,300 a day.”
“This isn’t worth $23,000 a day!” she shot back.
Dean, the facility’s owner, was nowhere to be found. On Tuesday, when Verdin heard that he’d yelled at an inspector from the state department of health, over the phone, telling her to stay away from the premises, she felt a new level of despair. If Dean can kick the state out, we’re doomed, she thought. Later that evening, an ambulance driver who had come to pick up a resident saw Verdin crying.
“What is going on here?” he said. “How long have y’all been here? I’ve never seen anything like this before.”
“Can you please get us help?” Verdin said. “Call somebody. Get us help.”
On Wednesday morning, five days after residents arrived at the warehouse, relief finally came. First Verdin noticed outsiders in the facility: Men wearing polo shirts and khakis, talking with the administrators. She knew they had to be from the state. An hour or two later, a colleague told her that ambulances and buses were arriving. She went outside to look, and they were already filling the parking lot, lining up far down the road: big, boxy charter buses with tinted windows.
Verdin started singing a song she remembered from church services she’d occasionally been taken to in childhood: “I’m So Glad Jesus Set Me Free.” She belted out the words while she helped prepare the residents to be moved.
It took all afternoon to load the hundreds of residents on the buses; Verdin’s residents didn’t leave until the evening. She refused to put her aunt on a bus, because no one knew where the residents were being taken. Late that night, the two caught a ride from a fellow nurse, and Verdin reunited with Ward, her partner, in the early hours of the morning.
The next day, as they drove to Houston, Ward tried getting Verdin to talk about what she’d been through. For one of the only times since he’d known her, she barely spoke.

Nursing homes raise thorny questions about disaster preparedness, not least because the usual prescription — asking people to remove themselves from the path of the storm — doesn’t really work in this context. As a result, deadly outcomes like those suffered at Dean’s operations are fairly common during major storms, though they tend to get limited coverage beyond regional news reports.
When nursing home residents shelter in place, all sorts of problems can arise. Their facilities can flood — as the St. Rita’s nursing home near New Orleans did during Hurricane Katrina, leaving 35 residents to drown in their wheelchairs and beds. Infrastructure can also break down. On balance, this poses an even larger threat than the direct effects of storms, according to research by David Dosa, a geriatrician and Brown University professor who has studied the effects of weather events on populations in long-term care. Power loss and the subsequent failure of air conditioners in particular can cause residents to die of heat exposure. This is exactly what happened to a dozen residents of a Florida nursing home during Hurricane Irma in 2017.
However, this doesn’t mean that evacuation is always a safer option. For those who are elderly and have chronic conditions, moving from a stable environment to a more makeshift one is risky. Vulnerable residents can die from heart failure, falling, or from illnesses like COPD being made worse by air pollution or shifts in temperature. Some health effects may not become apparent until days or weeks after the storm — and in those cases, they usually aren’t counted in statistics detailing storm-related deaths.
“I think we tend to spotlight these bad apples, and say, ‘How could we do this? How could we let this happen?’” Dosa said. “The reality is, you’re kind of damned if you do [evacuate], damned if you don’t. It’s a bad situation across the board.”
In 2020, Dosa and several of his peers published a sweeping analysis of mortality rates among Florida’s elderly population, comparing 2017 — the year Hurricane Irma hit — to 2015, when there were no hurricanes. They found that there were 262 more nursing home deaths within 30 days after Irma made landfall, compared to 2015. At 90 days, there had been 433 more deaths.
Careful preparation can mitigate the amount of harm — and climate change is making those preparations even more urgent. Empirical evidence suggests that the warming atmosphere is driving up the frequency of Category 4 and 5 hurricanes, though smaller hurricanes are happening less often. Multiple studies have also suggested that climate change is causing storms to undergo rapid intensification that can increase their unpredictability and severity, and that it’s adding to the amount of rainfall that accompanies them.
While the ways that climate change is threatening the U.S. long-term care population is still coming into view, it’s clear that the scale of the challenge is vast. In 2021 and 2022, well over 100 nursing homes and assisted living facilities were evacuated during named storms.
To the extent that many nursing homes have neglected these threats, the trend reflects a problem inherent in the industry and its funding structure, according to Richard Mollot, executive director of the Long Term Care Community Coalition, which advocates for better nursing home conditions across the country. Many of these facilities receive a large part of their funding from the federal government’s Medicare and Medicaid programs, which pay out set rates for each resident, regardless of the quality of care. This means that facilities are essentially paid in advance for their services, Mollot said, “and if they don’t spend it appropriately, there’s no clawback.” This gives facility owners like Dean an incentive to keep their overhead as low as possible, to maximize profits. While they must submit cost reports, these don’t have to be reviewed by certified accountants, Mollot pointed out, leaving room for “a tremendous amount of fraud.”
The consequences of such cost-cutting and unpreparedness have led Gulf states to strengthen disaster preparation requirements for nursing homes, as Louisiana did after Hurricane Ida, in an attempt to make sure facilities’ emergency plans are carefully reviewed before it’s too late. But as climate-driven disasters continue to pose unforeseen threats across the U.S., the lessons from the industry’s recent failures will only become more relevant.
Verdin began her nursing career in 2007, when she was in her early 30s and her four kids had all reached school age. In her family, which is indigenous to Louisiana’s Gulf Coast, it’s understood that the men are providers, she said, and the women don’t work. When she accepted her first job, her father and brothers staged what she described as an “intervention.” She couldn’t be persuaded.
“Well, I’m not going to worry about it,” her father said, “because you’re so hot-tempered, you won’t keep a job.”
She knew he was right about her temper, at least. Growing up in Cut Off, she’d been suspended from school again and again. She and her siblings were the only Native kids in their classes, and whenever someone called her a “Sabine” — a racial slur barely known outside of coastal Louisiana — her usual response was to start swinging.
“I never lost,” she recalled. “I fought boys, too. Girls, boys, the bus driver …”
But her tenacious personality would serve her well as a nurse. The first facilities where she worked were Raceland Manor and Maison DeVille, which were owned by Bob Dean. Though she’d never heard of Dean, he was widely known in the state capital of Baton Rouge, where he was legendary for collecting antiques and classic cars, and for his role in restoring the downtown district. He had purchased many buildings, including the city’s first skyscraper (built in 1912) and the 14-story Republic Tower, which he renamed Dean Tower. In 2002, he opened a downtown auto museum, with room enough to display 25 of his cars — roughly a third of his collection.

But if there was a disreputable side to Dean’s enterprises, it involved his nursing homes. During Hurricane Georges in 1998, he ordered that 300 residents be moved to a former bank building he owned, which wasn’t up to fire code. One patient died en route, in a bus that lacked air conditioning, and a diabetic patient reportedly died after being given orange juice and slipping into a coma. Local authorities weren’t notified until emergency calls started coming in.
Verdin noticed problems that were more chronic. The buildings were in poor shape, she said, with mold everywhere and holes in the ceilings. At Maison DeVille in particular, there were rats, roaches, and mice. “It stunk,” she said. When it rained, they had to put buckets and garbage cans around to catch the water.
Dean, who usually traveled in a private plane, made periodic visits to speak with administrators. But “he wouldn’t even walk in that facility,” Verdin said. “That’s how disgusting it was.” Instead, she remembers him meeting with the director outside or in a restaurant across the street.
The problems at Dean’s facilities were no secret. The Times-Picayune newspaper — which, since its merger with The New Orleans Advocate, has published dozens of articles on the disaster in Independence and its aftermath — reported in 2005 that five patients in Dean’s nursing homes had died because of inadequate care over the previous six years; his company had settled wrongful death suits in another seven cases. It also reported that a woman living in one of Dean’s homes was sent to the hospital with 500 bites from fire ants after her bed became infested.
These problems may have stemmed, at least partly, from understaffing. In recent years, according to federal records, one of Dean’s nursing homes in New Orleans had less than three hours of staff time per resident per day, putting it in the bottom 8 percent of nursing homes nationwide. Two others were in the bottom 17th percentile.
However, the state never intervened in any serious way — and this reflects a broader pattern with the Louisiana Department of Health. Between 2006 and 2021, according to the Times-Picayune, the department tried on only three occasions to revoke the licenses of nursing homes. None of those attempts resulted in permanent closures of the facilities. In one case, a federal judge overruled the department. Most of the state’s elected officials have not expressed much interest in creating a stricter regulatory culture — perhaps because many received large donations from the nursing home industry. Between 1994 and 2021, Dean alone gave at least $289,000 to political campaigns.
Despite her discomfort, Verdin continued working at Dean’s facilities. The money was good, and by then she was a single mother — her husband had left 11 years into their marriage. Her kids were becoming teenagers, and they were playing sports and taking driver’s ed. “That costs money,” she said. “And with no help, I did what I had to do.”
Besides, she felt that if she were to leave, she’d be abandoning the residents. In 2018, she took the job at South Lafourche. To her judgment, it was Dean’s cleanest and best-run nursing home, so she decided that Roussel, her aunt, would be safe living there under her own watchful eye. Roussel was intellectually disabled — “she was like a kid,” Verdin said — and for years, Verdin’s mother had been caring for her.
At first, Roussel thrived at South Lafourche. “She had a laugh that could just fill the whole room and have everybody cracking up,” Verdin said. She made sure Roussel had a superb care plan and received a bath every day.

Janice Verdin has worked as a nurse in south Louisiana for over 15 years.
Later that year, when Verdin arrived at work the morning after getting the text message that South Lafourche was evacuating due to Ida’s approach, there were already buses in the parking lot. Inside, the atmosphere was hectic, but her colleagues were in good spirits as they rushed around, packing food, clothes, and medical supplies. “I really just didn’t think it was going to be that bad,” recalled Helmer, Verdin’s colleague. “I thought we were going to be at the warehouse, like, two days, until the storm passed.”
As Verdin pitched in with the packing, however, she felt a sense of dread. She remembered the first time she’d gone through an evacuation at one of Dean’s facilities, in 2008, when she and her colleagues and the residents relocated to a former Winn-Dixie store near Baton Rouge. The amenities her boss had promised, like catering and childcare, didn’t materialize, and after a few days garbage was piling up all over. The state eventually declared the conditions uninhabitable.
Verdin warned her colleagues at South Lafourche to prepare for the worst. “Just so you know, y’all better bring some food,” she said. “Do not bring y’all’s families, ʼcause this is about to be bad.”
Evacuating nursing homes is inherently dangerous, because travel can be jolting for residents who are elderly and infirm. The federal government requires facilities to have detailed evacuation plans, and Louisiana has its own standards on top of those. However, there was a loophole, according to Denise Bottcher, the state director of AARP Louisiana: No one in Louisiana’s government was required to review those plans, once they were submitted. There was no mechanism for enforcement.
Had the state taken a closer look at the plans for Dean’s facilities, it would have found that the site he had in mind was a terrible place to send elderly patients. Though Dean described the building, on different occasions, as an “alternative care facility,” a former Fruit of the Loom warehouse, and a Febreze factory, in reality it had been part of a pesticide plant — and it was still under a cleanup order from the state, as of 2021, because the groundwater had been contaminated by dangerous chemicals. Regulators also failed to notice other shortcomings in Dean’s preparations, according to the nurses who worked at his facilities, which led to a failure to bring enough medical supplies when it came time to relocate.
Helmer believed that South Lafourche should have rented a U-Haul in the days before the evacuation to ensure that the warehouse was appropriately supplied — but she knew that her managers wouldn’t want to spend the extra money. After all, during normal months they wouldn’t even spend a few hundred dollars to cut the grass outside the nursing home. “It was always about the money,” Helmer told Grist. “It was cheap, cheap, cheap.”

On the afternoon of the evacuation, while Verdin was still in Cut Off, a state inspector visited the warehouse in Independence and noted that the building had an allowed capacity of 600, but 700 or more residents were scheduled to arrive. There would not be laundry or linen service for at least five days, the staff told the inspector, and the warehouse had no kitchen. On the paperwork, where it asked whether there was an “Adequate number of cots/beds/mats,” the inspector marked “No.”
Within a day after Hurricane Ida had passed over the warehouse, at least three patients had been taken to hospitals, and another 15 who were morbidly obese or had tracheostomies desperately needed to be placed somewhere else. As for Bob Dean, he never came near the warehouse. Around 6 p.m. on Monday evening, according to court records, he sent a text message to his employee Donise Boscareno, who was overseeing the operation. “How is everything going there?” he asked.
“It is not well,” Boscareno replied. “We cannot do this. We cannot take care of our people. People are dying. We need to send them somewhere they can be cared for medically.”
Dean suggested that she was having a “breakdown” and said he’d send over another supervisor to relieve her. “I do not want any more patients to leave that building,” he wrote.
A state inspector who visited the warehouse on Tuesday, four days after the residents arrived, confirmed that conditions had deteriorated: Garbage was piling up, and there were puddles of mud and water everywhere. One man “was in a T-shirt and a diaper that was full of feces,” she wrote. “There was a female resident softly calling for help and no staff could hear her. There was no way for the residents to signal to staff that they needed assistance in this sea of crowded together, cluster of mattresses on the floor other than yelling out for them. The nonverbal and softly spoken (in this loud gymnasium) would have to rely on staff checking on them.”
The inspector returned later that same afternoon, state records show. A staffer put her on the phone with Dean. She said she worked for the Louisiana Department of Health, but this didn’t satisfy the entrepreneur.
“Who sent you?!” he yelled again and again, continually interrupting the inspector as she tried to respond. She suggested he call her supervisor, but he would only repeat, “Who sent you?!”
“When I responded one last time I would not answer that question he said, ‘Get off my property! Now!’” she wrote in her report. She gathered her belongings, called a colleague to report what she’d seen, and left. The next morning, the residents were finally removed from the warehouse.
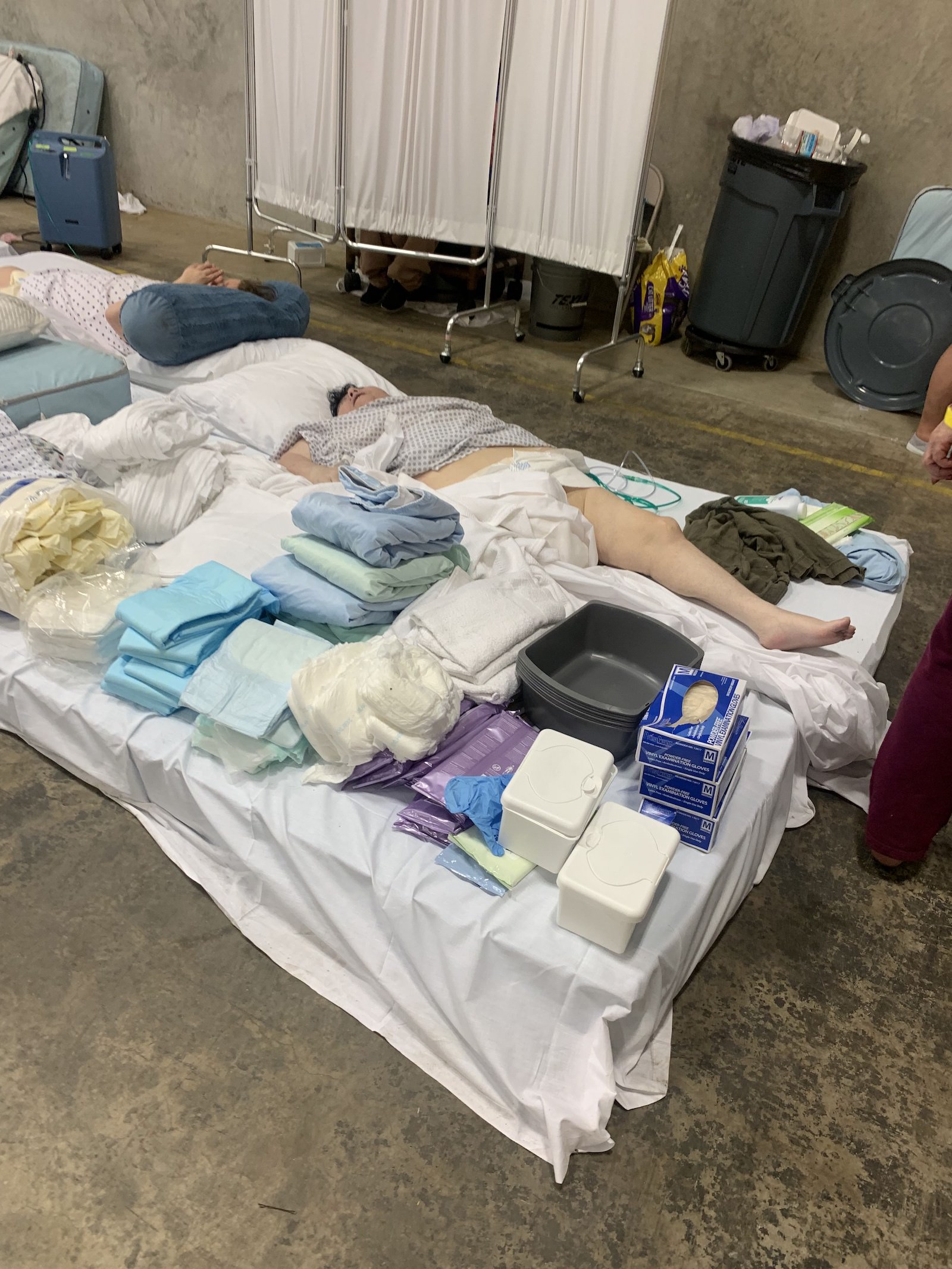
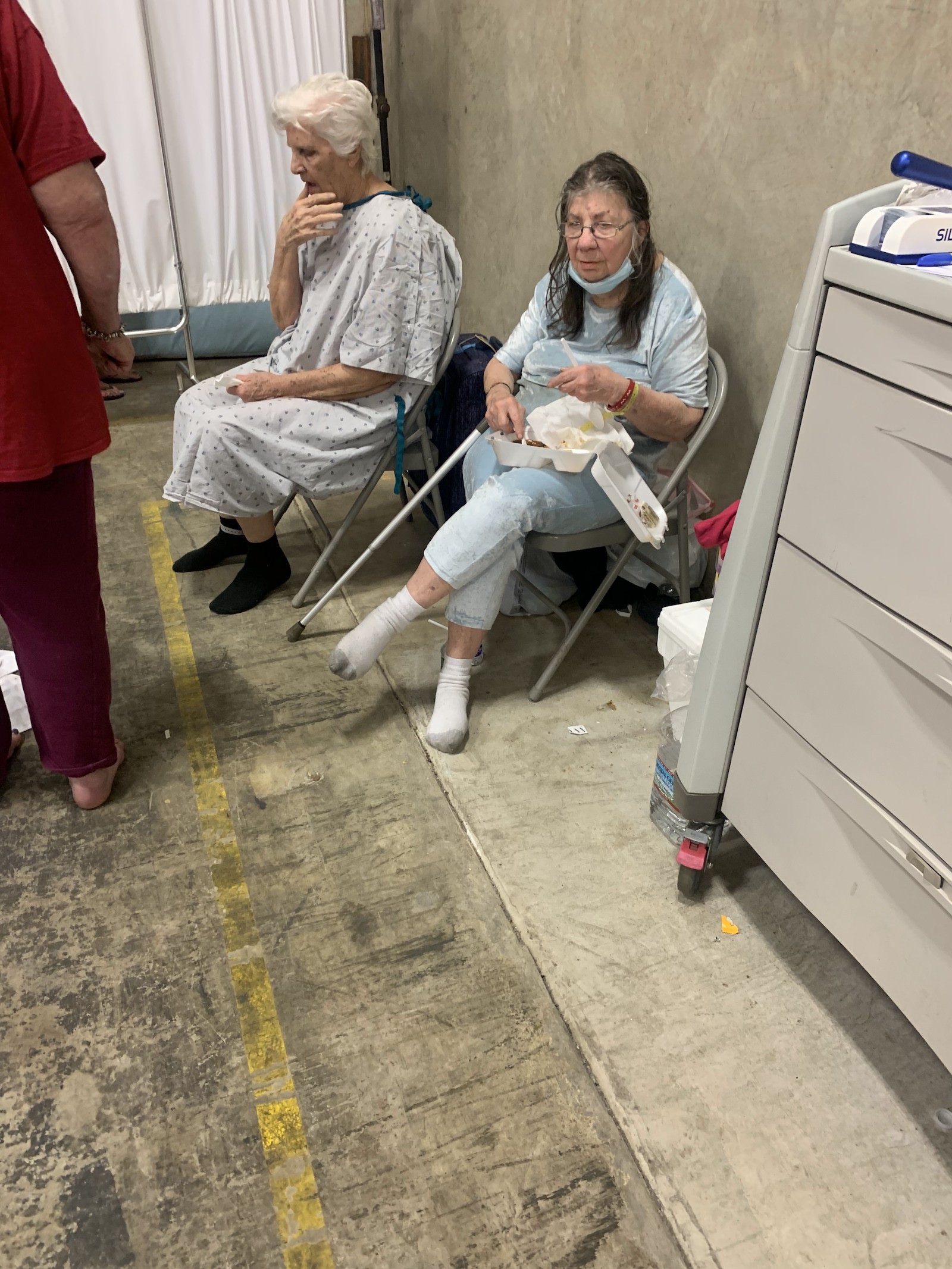

Conditions rapidly declined inside the warehouse, where there was no laundry service or a kitchen. A state inspector who visited the warehouse marked “No” on paperwork that asked whether there was an “adequate number of cots/beds/mats.” Janice Verdin
A few days after Verdin and her aunt had safely left for Houston, Verdin called Don Massey, an attorney she knew in New Orleans. He’d already heard about the warehouse debacle in the news. “Janice, how did you get mixed up into this?” he asked.
On the following Monday, the courthouse was closed for Labor Day, but Massey faxed a legal complaint to a judge — he didn’t want to waste any time. In the document, he accused Dean and his lieutenants of creating “horrific and inhumane conditions” for nursing home residents and said they had violated the state’s Nursing Home Residents’ Bill of Rights Act. It was a class action suit, filed on behalf of Verdin and three other people whose relatives had been part of the evacuation. Many residents’ family members, he wrote, were still trying to figure out where their loved ones had been taken.
The very next day, the state announced that it was revoking Dean’s licenses for all seven of his facilities. This meant Verdin and nearly 1,000 other employees were out of work. Dean told local reporters that he had a deal in the works to sell all seven nursing homes — he stood to make around $70 million — and a broker estimated that the licenses alone could be worth $1 million per building. Dean remained defensive, saying that four of the residents who had died had already been on hospice care, and at least one more had died of natural causes. He didn’t know why the state officials had been so alarmed by conditions at the facility.
“To get right down to the point, I don’t know, bureaucrats think and do things differently,” he said. “They flip out.”
That same week, Dean moved swiftly to shield his money from the lawsuit, the federal government would later charge. He berated his bookkeeper, yelling and screaming that she should “sweep” all of his businesses’ financial accounts. Some accounts had already been frozen, but the bookkeeper successfully moved $877,000 into Dean’s personal account, according to the government’s allegations. He also went on a buying spree, spending $1.75 million on antique firearms and $100,000 on a luxury car. He also used a business account to pay down personal debts and to make cash gifts to his wife and stepchildren.
Other misdeeds on Dean’s part would soon emerge. The Department of Justice would report that in the years leading up the evacuation, Dean had illegally pocketed $1 million that his nursing homes paid in “rent” for the warehouse — money that was supposed to be used for improvements, including disaster preparedness, as a condition of the federally backed loans he was receiving. A legal filing also charged that he’d violated residents’ rights by not revealing that the warehouse had once been part of a pesticide plant.

A few months into the court proceedings, Dean’s attorneys filed paperwork saying he had dementia and wasn’t fit to testify. Former colleagues testified in depositions that they had noticed changes in his behavior during the months leading up to the evacuation: One said Dean would slur his speech and drool all over his shirt without noticing it.
Verdin, for her part, didn’t mind being temporarily out of a job. The lawsuit consumed her. For the first month, Massey was the first person she spoke to every morning and the last person she spoke to each night. The suit he filed was merged with several others — including one filed by Morris Bart, an attorney known throughout several Southern states for his billboards (“One Call, That’s All!”) — into a class-action case. In the end, roughly 400 plaintiffs signed on.
But as the court proceedings moved along, their hopes for a major settlement quickly dimmed. Massey learned that Dean was deep in debt: He owed more than $96 million to various creditors. A Baton Rouge bank that had loaned him $10 million shortly before the hurricane was allowed to seize 28 of his classic cars as collateral, according to court records first reported on by the Times-Picayune. It became clear that the best outcome family members could hope for was a swift payout from Dean’s insurance policies, which would max out at $12 million to $15 million in total.
In November 2022, only 14 months after the evacuation, a judge approved a settlement for $12.5 million. The early estimate was that, after attorneys’ fees, most families would receive less than $10,000.
In an email to Grist, J. Garrison Jordan, an attorney representing Dean in the ongoing criminal case against him in Louisiana courts, wrote that Dean “adamantly denies the allegations” against him. He “maintains his innocence,” Jordan wrote, “and looks forward to defending himself in a court of law where he looks forward to vindication by a jury of his peers.” Meanwhile, the federal government is also suing Dean on accusations of financial misconduct.
The state of Louisiana, for its part, has learned a few lessons from the events during Ida. Last year, with input from Denise Bottcher of the AARP and other advocates, the state health department established new requirements for “unlicensed” evacuation shelters, such as churches, gymnasiums, and auditoriums. Every site now has to provide at least 60 square feet per person, adequate ventilation, and a working air-conditioning system, along with a minimum number of showers, sinks, and toilets. The department has also started requiring that every nursing home’s evacuation plans be rigorously reviewed and kept up to date.
Bottcher is cautiously optimistic that events like the one in Independence won’t recur in future storms. Still, she said, many Louisianans are wary. “There’s just not a lot of trust,” she said, ”that the department will do what it says it’s going to do.”
Since 2022, Verdin has been working as a contract nurse instead of taking a staff job. She keeps in touch with a few colleagues from Dean’s facilities, but for the most part, she feels like a pariah. After all, she was part of the process that led to the nursing homes being shut down and her colleagues needing to find new jobs.
The death count, within a month after the storm, was 15. Other residents suffered permanent injuries, including at least two who developed gangrene and had their legs amputated. But this official count doesn’t include people who died later from illnesses apparently related to the evacuation.
Ultimately, Verdin’s aunt was among the casualties. When Roussel and Verdin first left the warehouse, Verdin said, her aunt seemed fine; but as the days went on, Verdin noticed that she wasn’t herself. She tested positive for COVID, and after several weeks of declining health she died at the end of the month. She was 65.

Even though she did everything she could for Roussel, Verdin is sometimes wracked with guilt, because it was her idea to bring her to South Lafourche in the first place. She has no idea how many others contracted COVID at the warehouse. But as of early 2023, 147 of the evacuated patients had passed away.
Verdin had been seeing a therapist well before the evacuation, but she didn’t feel ready to discuss the experience in any detail in her sessions for months afterward. Finally, around December 2021, she recounted everything over the course of an hour. By the end, she had a crushing headache and was sick to her stomach. It’s easier for her to discuss it now, but the experience still haunts her.
Sometimes she daydreams about starting a new career, as an advocate for nursing home reform on Capitol Hill. “If you tell me I could bring change,” she said, “I would probably do that for free.”








